More than just convenient. It’s clinically proven.
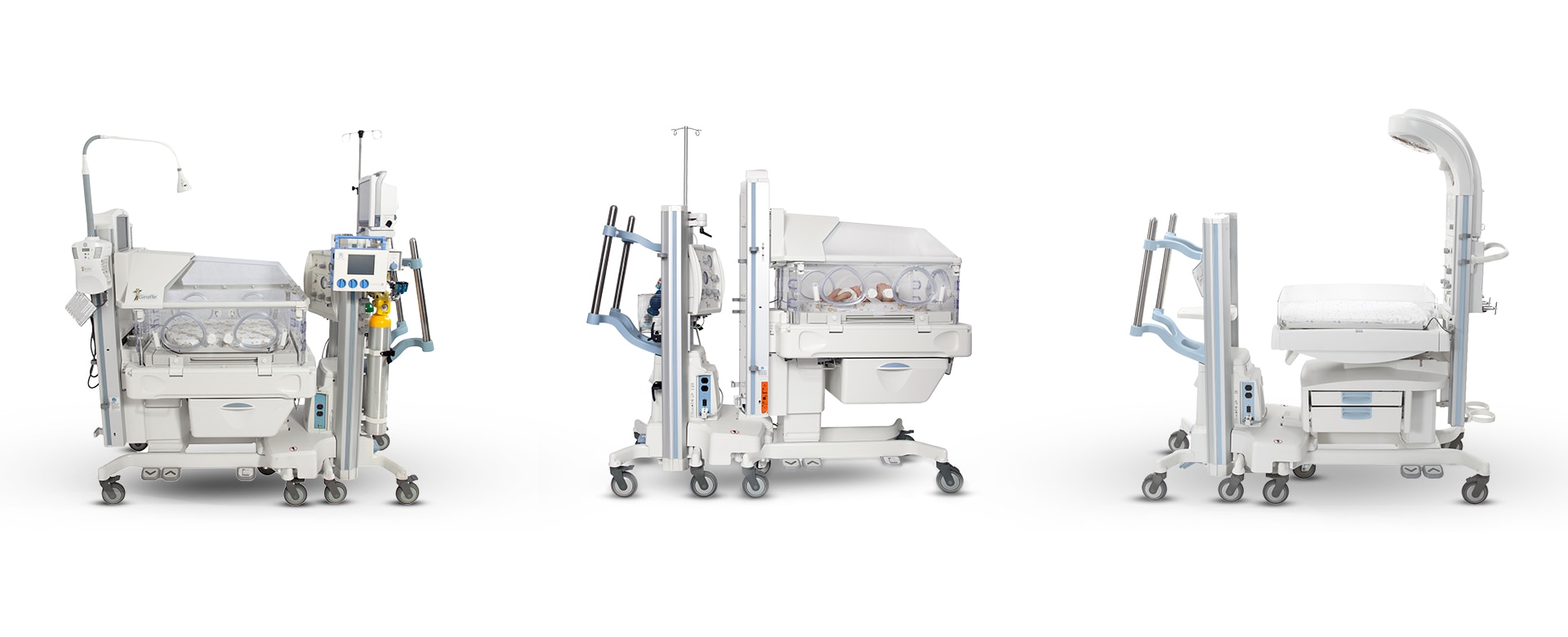
Helping you create a safer transport environment for neonates means a better bottom line.
- Bed transfers contribute to lower admission temperatures5,6
- Lower admission temperatures contribute to higher infection rates7
- Infection treatment leads to higher cost8
How-to Videos for Giraffe Shuttle
Giraffe Shuttle motion
Giraffe Shuttle product side
*Incubators and warmers compatible with the Giraffe Shuttle include: Giraffe OmniBed Carestation, Giraffe Incubator Carestation, Giraffe Warmer, Panda Warmer, Giraffe Incubator and Giraffe OmniBed
1. https://www.sciencedirect.com/topics/medicine-and-dentistry/neonatal-transport - W. Alan Hodson, in Avery's Diseases of the Newborn (Tenth Edition), 2018
2. http://ccn.aacnjournals.org/content/30/4/18.full. Are you satisfied with your outcomes? Or do you feel they can be better?
3. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4966347/
4. Kim SM et al. Improved care and growth outcomes by using hybrid humidified incubators in very preterm infant. Pediatrics 125(1), 137-145, 2010
5. Nedrelow J, Bloom BT, and Clark RH. Admission temperature is an independent predictor of survival for infants born between 24-29 weeks gestation. Pediatric Academic Society Meeting, 5/7/2007, E-PAS2007:617934.25.
6. Bhatt DH, Carlos CG, Parikh AN, White R, Seri I, and Ramanathan R. Prevalence of transitional hypothermia in newborn infants on admission to newborn intensive care units. Pediatric Academic Society Meeting, 5/7/2007, E-PAS2007:617933.23. • From 24 to 29 weeks…temperature had an independent effect on survival. For each degree change there was an increase in survival by approximately 10%.
7. Laptook AR, Salhab W, Bhaskar B and Neonatal Research Network. Admission temperature of low birthweight infants: Predictors and associated morbidities. Pediatrics 2007; 119:e643-e649. • Admission temperature was inversely related to…late-onset sepsis (11% increase per 1°C decrease).
8. Payne et al , 2004. Marginal Increase in Cost and Excess Length of Stay Associated With Nosocomial Bloodstream Infections in Surviving Very Low Birthweight Infants, Pediatrics, Vol 114, No2. • Nosocomial Infections have the greatest impact on overall cost for very low birthweight Infants.
9 F. Loersch, M Schindler, K. Starr of GE Healthcare, J. Moore, L Lynam Bayne. “Risk Factors for intra-hospital transport of newborn patients: A new solution to an old problem”. Journal of Neonatal Nursing (2011) 17, 203-214
10. Snug as a bug. Evaluating thermoregulation capabilities of newborn hybrid incubators based technology, testing and track record, white paper
11.Viera ALP, N. do Santos AM, Okayama MK, Miyoshi MH, de Almeida MFB and Guinsburg R. Factors associated with clinical complications during intra-hospital transports in a neonatal unit in Brazil. Journal of Tropical Pediatrics, 12/2010
